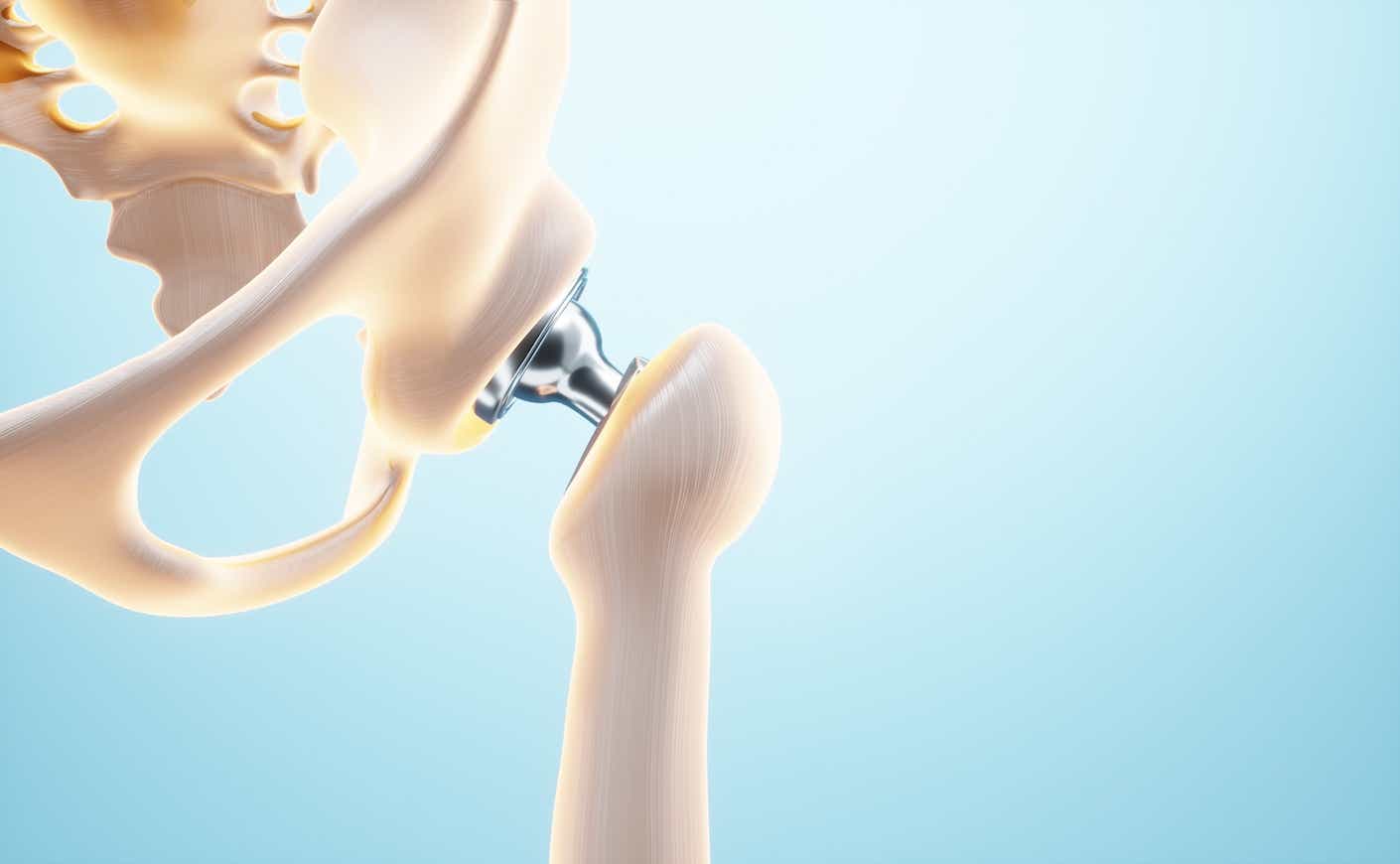
It’s a harsh but undeniable truth that our bodies will suffer a little wear and tear over time. We’ve all gotten used to a few extra creaks as the years go on — but some of these changes can be hard to live with, especially if they’re accompanied by debilitating pain. One of the more common (and most inconvenient) of these developments is issues with our hips. The good news is that, in some cases at least, there’s a (relatively) simple solution.
Between 2012 and 2018, 602,582 total hip procedures were reported to American Joint Replacement Registry. Last year, the iconic matriarch of the Kardashian clan, Kris Jenner, joined their ranks — and of course, she generously documented her entire experience on The Kardashians.
Jenner had suffered serious hip pain, even telling her doctor that she "literally couldn't walk" across a room without a cane. You might be able to relate to that experience.
Despite some heartache over what a hip replacement might signify — she admitted that the prospect of surgery was “scary,” and made her feel “older than I feel on the inside” — she decided to take the plunge. Afterward, she couldn’t conceal her glee at the speed of her recovery.
"I'm so excited just to get back to the office on a regular basis, get back to playing with my grandkids, giving Corey a little more attention…if you know what I mean," she beamed wickedly.
At the time, Jenner was almost the exact average age of hip replacement patients (which is 67). But what if her now-27-year-old daughter Kendall needed the surgery? Or her 88-year-old mother, Mary Jo Campbell? Can you be too old to go under the knife, or too young? We asked top orthopedic surgeons to give us the score — and whether, when it comes to hip pain, it’s better to wait and see, or embrace your inner “bionic woman.”
First off, can you be “too old” for a hip replacement?
The short answer? No. There’s no cut-off point when you become “too old” for surgery — though, as Lee Rubin, MD, an orthopedic surgeon at Yale Medicine explains, there are a few more risks to weigh. An older patient’s bone quality or bone density around the hip when the implants may be placed is likely to be more fragile, which can lead to early loosening or fractures after surgery.
“For the truly elderly” — that’s patients in their 80s, 90s, and even those more than 100 years old — “doctors become more concerned about potential illnesses around the time of the surgery and during early recovery,” says Dr. Rubin.
These patients are at a higher risk for cardiac and pulmonary complications and can develop pneumonia, stroke, or even kidney failure after the operation. Because the over-80s have a slightly higher mortality rate after hip replacement surgery than younger patients (about 1.5 percent, versus 0.5 percent for those aged 70-79), their healthcare team should be especially vigilant to keep them safe following the operation. That being said, it’s very common for people in these age brackets to undergo hip replacements — and the prognosis tends to be very positive.
“In general, even for these most elderly patients, the outcomes of hip replacement surgery with regards to pain relief, hip function, and range of motion, are the same as any younger patient,” says Dr. Rubin. “Our research here at Yale on joint replacement in the elderly has shown that there’s an increased risk for hospital readmission, but there’s not typically an increased complication rate related to the surgical procedure itself.”
The evidence, Dr. Rubin says, indicates that the benefits of hip replacement surgery tend to outweigh the risks. In the overwhelming majority of cases, patients are delivered safely through surgery.
“In fact,” he adds, “I completed a hip replacement this morning on an 86-year-old, who is resting comfortably and is expected to do great in their recovery process!”
Should younger people wait for hip replacements?
Hip replacement is typically suitable for patients with severe degenerative hip disease, and while this usually occurs after the age of 50, younger people can develop the condition, too. In the past, orthopedic surgeon Robert J. Avino, MD, explains, surgeons advised younger patients against surgery as the joint replacements would wear down over time — especially if the young person was very active. These days, however, things are looking up.
“More durable implants have been developed over the last two decades,” explains Dr. Avino. “By using advanced technologies like robotics, surgeons can place components more precisely, which decreases the rate of wear. Components that used to only last 10 years are now lasting 20-30 years, if not much longer.”
When Dr. Avino discusses potential hip replacement surgery with younger patients, they always consider how their day-to-day life is being impacted by their joint disease. “It’s a risk versus benefit decision,” he says. “To substantially improve quality of life, patients typically accept the small increased risk of additional surgery in the future for the immediate benefits of joint replacement.”
What if you’re in your 50s or 60s and you’re pretty sure you will need a hip replacement at some point — should you take the plunge now?
At the end of the day, you are the only person who can really judge how much your joint pain or dysfunction is interfering with your quality of life. “When a person crosses that line from tolerable to intolerable symptoms is a very personal decision,” says Thomas Hickernell, MD, a colleague of Dr. Rubin’s at Yale Medicine. “So, patients can wait for as long as they want to, but one of the most common things I hear from patients after their hip replacements is ‘I wish I hadn’t waited so long to do this.’”
It’s easy to unconsciously acclimatize to pain or inconvenience over time, so you might not realize how much independence your hip issues have cost you until after they’re fixed.
“I always think it’s worth trialing non-operative treatments for joint pain before committing to surgery because sometimes patients can get good relief for extended periods of time,” says Dr. Hickernell. (Non-operative treatments can include pain relief shots and physical therapy.) “But once a patient has reached a point where their daily quality of life is suffering, they can’t do the things they want to do anymore, and non-operative treatments are no longer helping, then it’s time to have a serious discussion with their surgeon about joint replacement.”