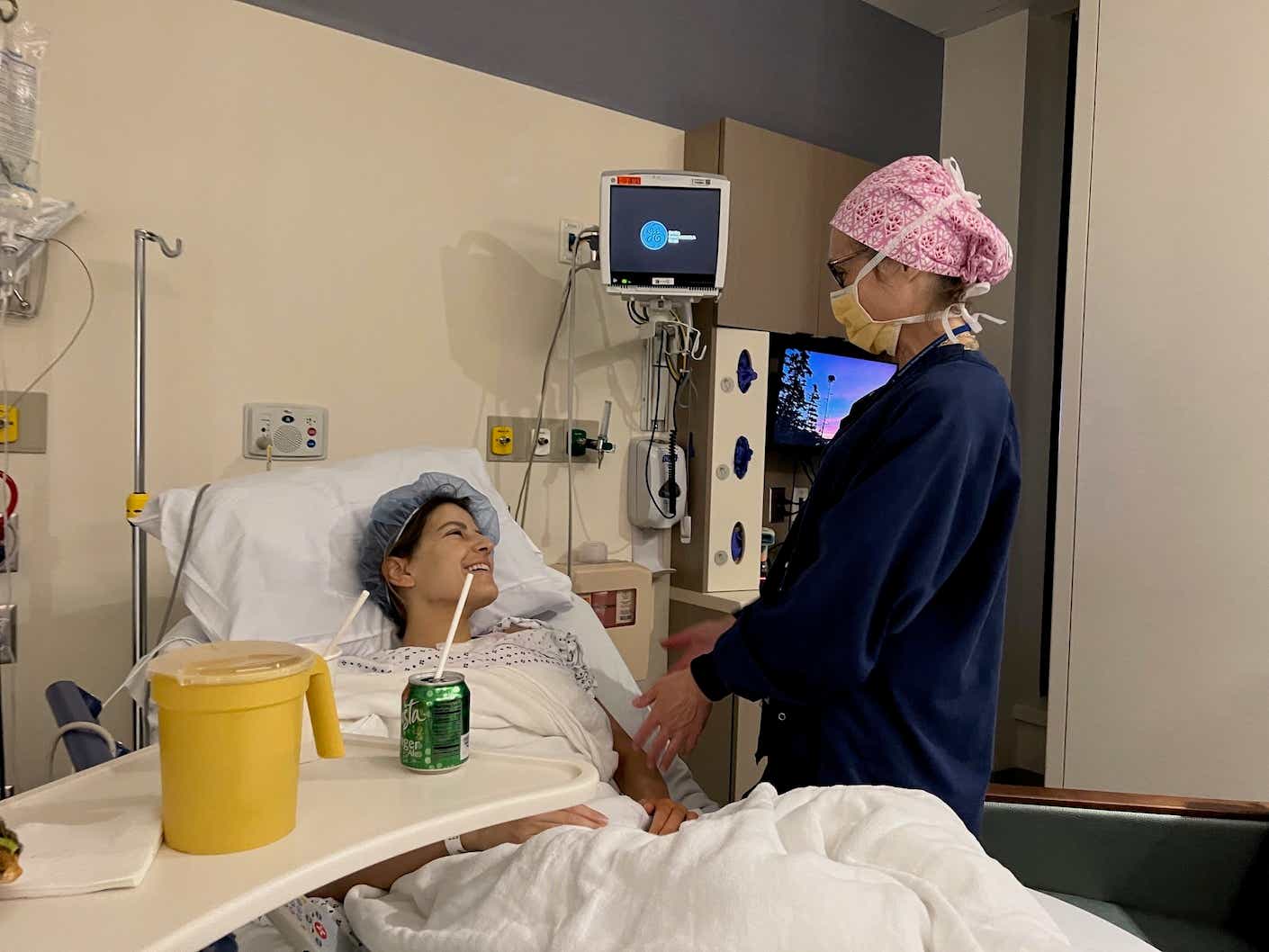
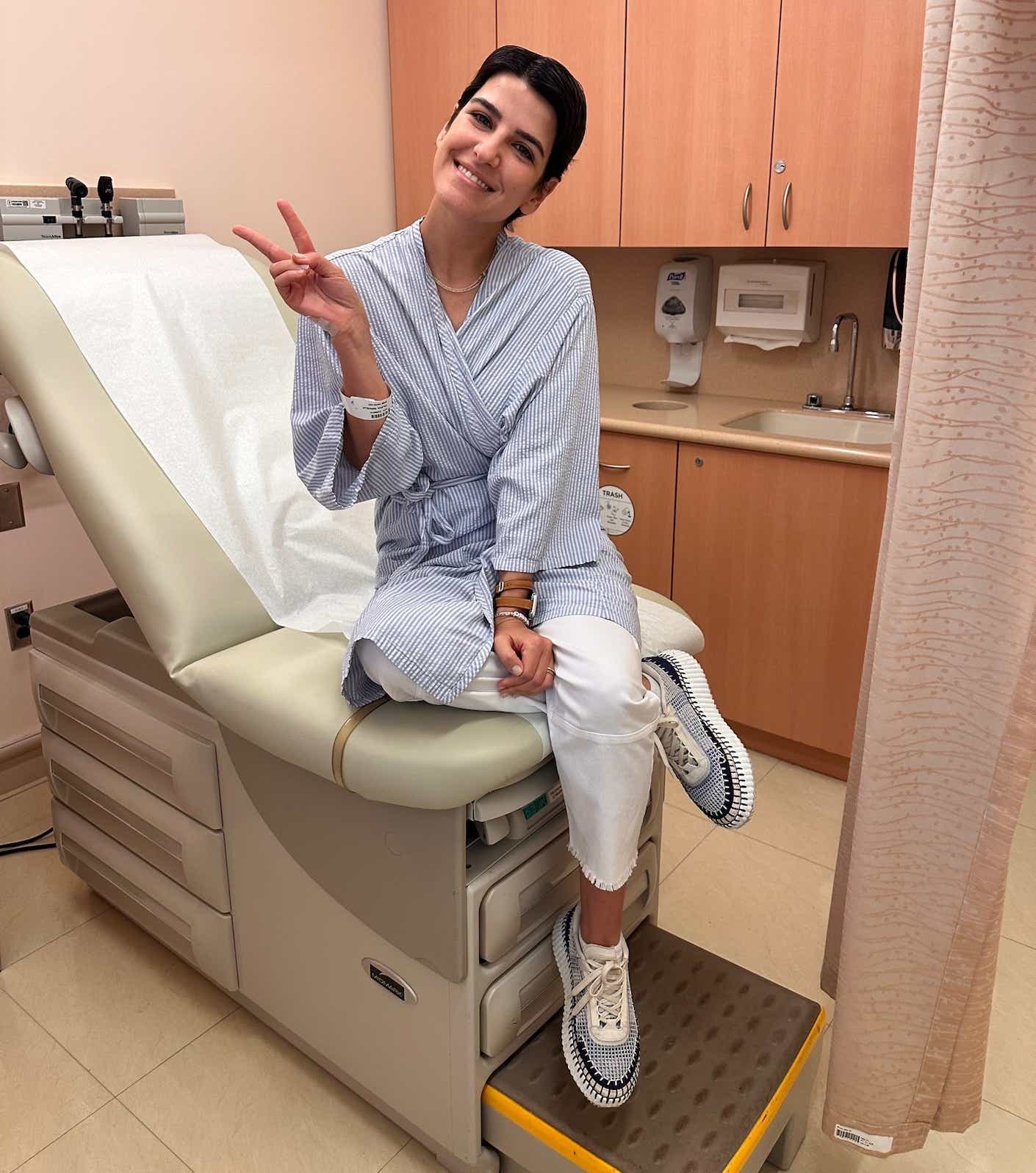
What were you doing in your 20s? Rushing to clock out of your entry-level office job so that you could go dancing with your friends? Getting back together with your ex for the third time? Noshing on ramen noodles to save up for rent (or concert tickets)? Giving yourself ill-advised bangs in your bathroom mirror? Young adulthood is supposed to be a time for exploration and carefree fun, but for some women, it means the unthinkable: Dealing with a breast cancer diagnosis.
The median age of a breast cancer diagnosis is 62. But unfortunately, many young women are faced with that devastation long before that — and even long before they reach the recommended mammogram screening age of 40. In fact, a recent study found that — from 2010-2019 — diagnoses of breast cancer among people aged 30 to 39 increased 19.4 percent. Among those aged 20 to 29, the increase was 5.3 percent.
We spoke to four breast cancer survivors who were diagnosed between the ages of 24 and 36 to understand the emotional toll of receiving a breast cancer diagnosis so young. They talked about everything from raising kids during chemo to shopping for wedding dresses without hair. These women visited the strange and terrifying world of “Cancerland,” and agreed that surviving breast cancer made them “the luckiest member of the sh*ttiest club ever.”
Discovering breast cancer
In August of 2022, Marcella Kelson, then 35, was on a much-needed getaway with her husband to Connecticut. The pair had their hands full with a four-year-old and a four-month-old at home. While riding in the passenger’s seat, Kelson took the opportunity to give herself a breast exam. “I’d had a physical breast check at six weeks [postpartum], but I always did self breast checks, too,” she says.
When she felt raised tissue on her left breast, she thought it was unusual but comforted herself with the promise that there was probably a reasonable explanation: “There are so many breast changes when you're recently postpartum that I thought maybe it could be a clogged duct.”
Abbie Marshall, then 35, found herself in a similar scenario when she was postpartum, and suspected the same. “I had recently stopped breastfeeding my daughter, and I thought I’d gotten a clogged milk duct. I reached out to a doctor to start antibiotics because I was worried about getting mastitis. But after a few days on antibiotics, [the lump] wasn't getting better.”
Lara Murphy, then 36, also mistook her lump for something less sinister than a tumor. “In college, I'd had some benign cysts that just went away. But this lump was not going away. I gave it a week or so to see if it changed with my cycle and it didn't. So I called my gynecologist, who said, ‘I have time right now. Can you come?’”

Since Sloan Robinson, then 24, had a family history of breast cancer, she asked for an assessment of a lump at her annual Well Woman checkup. “Both my grandmothers had breast cancer,” she says. “My mom and I had been talking about getting gene testing done for years, but we were scared to do it. So it was on my mind.”
But Robinson’s doctor pushed back. “My doctor told me that I didn't need to worry about it and that there was nothing wrong because I was 24. I said, ‘Can you just give me an ultrasound or a mammogram or something?’ She fought me on it. She said, ‘You don't need one. It's going to cost a lot of money.’” Robinson insisted: “I don't really care if it costs money — I'd rather get it for peace of mind. I know something isn’t right with my body right now.”
“It was ridiculous to say, ‘It’s expensive’,” Robinson says. “It's my body. If I didn't advocate for myself, by now I’d have stage four cancer.”
No matter what the response from the doctor, the diagnosis — however delivered — was a shock for all of these women.
Kelson’s OB immediately sent her for a mammogram and an ultrasound. When a radiologist referred her for a biopsy, Kelson expected to receive results later in the week. But the way she heard the news was less than ideal. “I got a MyChart update via email, and it said, 'Check in for your oncology appointment tomorrow.’ I thought, What the f*ck? I called the hospital and asked, ‘What's going on?’ Eventually, I got a hold of the radiologist and she told me that I was diagnosed with a breast cancer type called triple negative — which means that there were no hormone receptors attached to my tumor. It’s a cancer that’s most often found in women under 40, and it’s the most aggressive subtype.”
For Murphy, it felt like she was quickly shuffled into what she calls “cancer orientation” at Duke Hospital, a short drive from her home. But despite the relief of her doctors taking her seriously and moving swiftly, the news certainly wasn’t good.“The urgency was terrifying — I was in shock. I thought, How do I tell everybody? I was a very healthy, active 36-year-old and nothing like this had ever happened to anyone I knew. I was alone in that.”
Finding community was easy, hard, funny, weird, sad, and impossible — all at once
Because most of the other patients battling breast cancer were decades older, these four women struggled to find peers who understood their situation.
“There's such a big emphasis on childhood cancer,” says Robinson, “But when you're not a kid but you're also not older, people seem to think, ‘Oh, you can't get cancer.’ It was very hard to find other people my age who were going through that.”
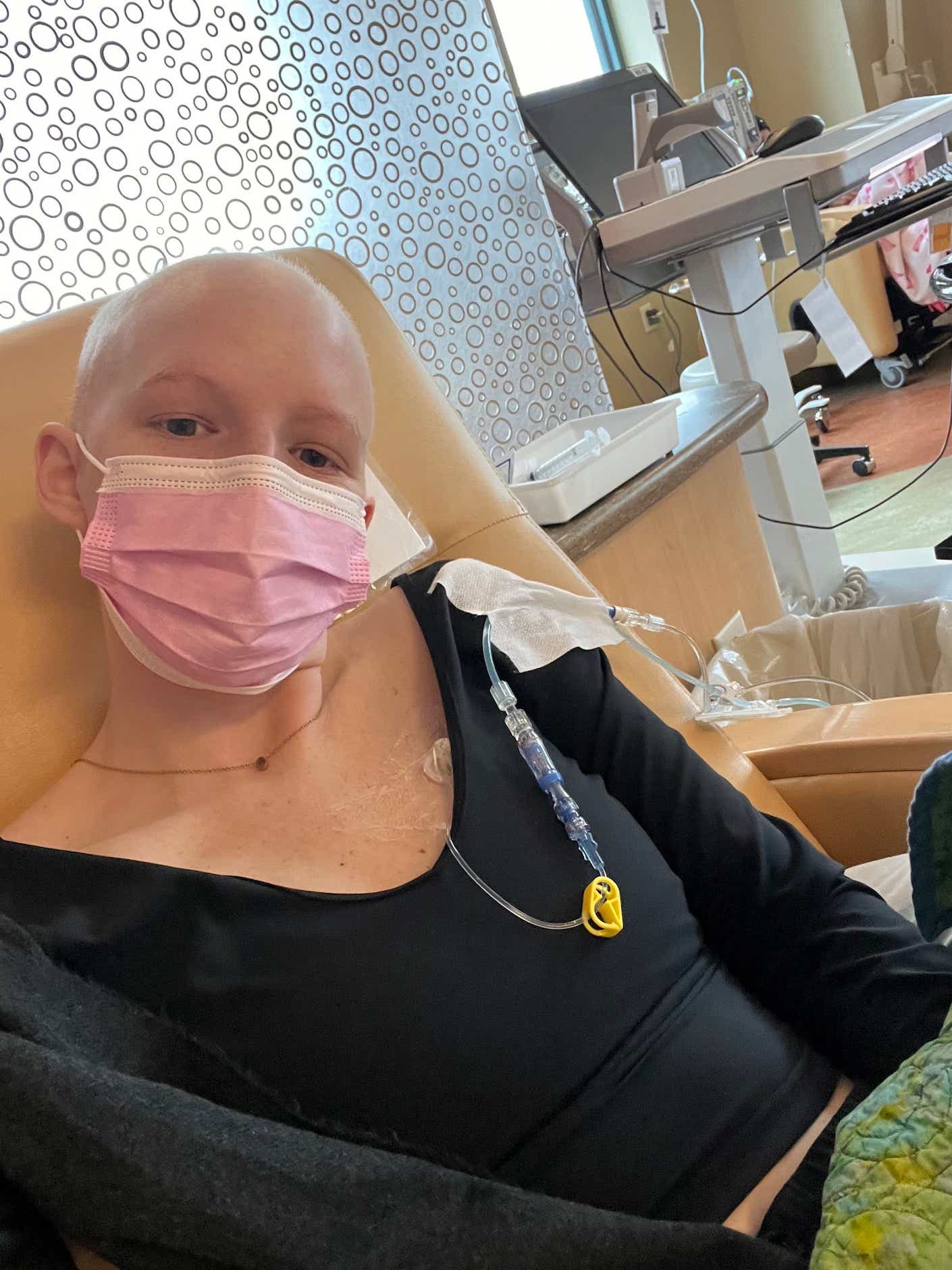
“My hospital connected me with a ‘peer’,” Robinson says, “but the closest they could find was a 34-year-old woman who had a different type of cancer. I'm part of some breast cancer organizations and I'm a spokesperson for one, but I'm the youngest by 20 years.”
Thankfully, Marshall found a support network: “Within days of my diagnosis and sharing the news, family and friends connected me to a handful of other young women around my age with breast cancer — a few other young moms who had recently gone through it, or were currently going through it. That made me feel less alone.”
Treatment sucked — but it wasn’t always what you’d expect
Chemo, radiation, surgery, and other treatment options aren’t known for being particularly fun. But these women challenged themselves to have a good time while they struggled, which they say was key.

Marshall tried to keep the experience as lighthearted as possible. “Each chemo treatment day, I would have an early morning Zoom dance party,” she says. “My friends and family would dance it out with me before most of them had even had coffee.” Marshall didn’t stop there. “I could have one person come with me to treatment, so for each one, I made a different theme: We did ones like superheroes, 80s prom, 90s workout, early 2000s, and pop star divas. It was silly, and it brought me joy.”
Robinson also tried to breathe some life into her treatment experience. “Cancer is nothing like the movies,” she says. “Movies make [the experience] seem a little bit worse and a little bit better than it is. My surgeon who did my mastectomy told me, ‘Don't think too much about chemo. You're young. You're going to be OK.’ That really shifted my mindset. I skied more than I've ever skied in my life on chemo. Everyone says, ‘You must have had such a bad year.’ It wasn't fun, but it also wasn't the worst year of my life.”
But Kelson grappled with the everyday challenges of motherhood in the midst of battling the disease. “My roles outside of breast cancer still existed even after I was diagnosed,” she says. “So I had to be thinking about my kids' activities and what they were going to eat that week while getting treatment.”
“I have a long life ahead of me — I'm going to be worried about recurrence.”
The lifelong threat of recurrence
Murphy recently received a clean scan; her body hasn’t shown evidence of the disease for seven years. She’s always willing to help or advise women who are recently diagnosed, but she’s also not going to sugarcoat the experience. “It's a very scary, expensive, painful, identity-destroying, body-destroying mind fuck,” she says.
Kelson celebrated her last immunotherapy round in September; now, she’s writing a children’s book aimed at helping kids understand a loved one’s diagnosis. “I found it challenging to be able to explain a lot of these things to my kids,” she says. “Being a young parent in this situation is very strange.”
Marshall, who just had her final breast reconstruction surgery, says she feels lucky that she was able to find so many resources and connections during such a challenging time. “I try to pay it forward since so many amazing women helped me in the early days of diagnosis,” she says.
Now 25, Robinson finished radiation last month. She’s looking forward to getting married next summer, even though cancer has heavily influenced her vision. She is still reeling from all the ways cancer has changed her, and has seen that seep into her wedding planning. “I had a mastectomy. It’s very hard to go through that as a 25-year-old — I lost one of my boobs. I also lost my hair. I'm going to try on wedding dresses this weekend, and I feel like a different person.”
Robinson says that to her, there is no “after.” “People think that cancer treatment is chemo and that's it, but it doesn’t end there,” she says. “Cancer has changed everything,” she explains. “I can't have kids without doing IVF. I'm going to have to constantly get mammograms and scans to make sure that I'm not having a recurrence. I have a really long life ahead of me in which I'm going to be worried about recurrence. I don't think everyone views cancer as a lifelong disease, but I definitely do.”
That said, she wonders if she’s been given this unique set of challenges for a reason.
“I feel like this is the reason I got breast cancer so young and am going to survive: If I can help one person figure out they have cancer, that would be a dream.”
Read this if you want to better understand why more younger women are getting breast cancer these days.