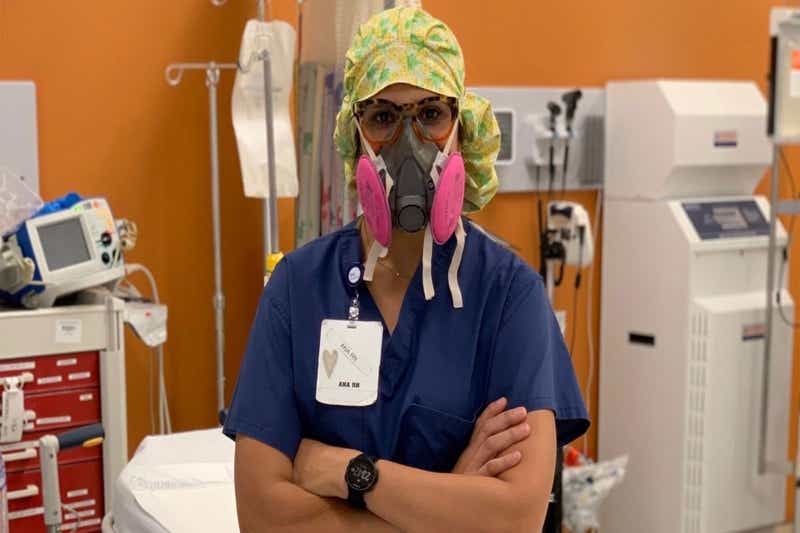
“We are just sort of doing MacGyver.”
As a veteran nurse, Ana Wilkinson is no stranger to emergency room care. Wilkinson has been working in emergency medicine for 15 years — this includes ten years as an ER trauma nurse and five as a paramedic EMT. She also took medical missions to developing countries like Haiti and the Dominican Republic — trips she described as being a “reset” button for her both personally and professionally. But nothing could have prepared her for what she would face after flying across the country to volunteer at a hospital in New York City.
Shortly after arriving from San Diego, Wilkinson said she was overwhelmed by the sheer number of Covid-19 patients — on her very first day she had 15 patients at once.
“I was shocked by so many people on the gurney,” she said, before adding that she was scared from what she did not expect.
Then there was a lack of medical resources, which Wilkinson says hasn’t improved as people continue to pour in. The hospital is still limited on a number of things like monitors, O2 stats and oxygen. “We are just sort of doing MacGyver,” Wilkinson said, referring to the beloved character who starred in the popular TV series of the same name. Like nurses today, MacGyver is known for his extraordinary knack for solving unconventional problems and saving peoples’ lives.
Wilkinson also didn’t feel confident in the personal protective gear that the hospital had provided, saying hospital workers were told to make their N95 masks last for five days due to shortages. Luckily, Wilkinson had brought some masks from home — and also ended up asking her husband, a firefighter, to send additional masks.
Like many Americans, Wilkinson had been caught off guard by the pandemic. Her family had been looking forward to going camping, and they had saved up for Disney cruise before the coronavirus derailed those plans. But since she had already taken the month of April off, Wilkinson decided to join the call along with many other nurses and doctors to battle the unexpected surge of Covid-19 cases in the nation’s burgeoning epicenter. Wilkinson contacted an agency to volunteer on the front lines, and two days later, she was at Harlem Hospital Center.
She said the most difficult part was breaking the news to her two young boys, ages eight and six. “The hardest thing for me was to tell my kids that, ‘Hey, I’m going to go to New York City,’” Wilkinson said. “I think it was different from saying like, ‘Hey, I’m going to Haiti or I’m going to Nepal.”
The experience has taken a toll on Wilkinson emotionally, but she finds strength in her family. Her two young boys hid letters in her suitcase, so every time she opens it, she finds another one. Her husband calls her every morning after she gets off from her night shift at the hospital. “I remember calling him on the first day when I was at Harlem and he’s like, ‘How’d it go?’ And I said, ‘Oh my gosh, I don’t know if I can make a difference,’” she recalled. “And he’s like, ‘just be yourself — just be Ana and you will.’”
Wilkinson is acutely aware of the importance of family when it comes to her patients. Given how highly contagious the coronavirus is, many patients aren’t able to see their loved ones in-person or feel a familiar touch before they die. Wilkinson said the hospital staff, in effect, becomes their family. “We hold their hand, we stroke their hair,” she said, adding that she finds comfort in knowing that she gave them “some feelings of love before they passed.”
Establishing a personal connection with the elderly patients who come into the hospital is especially important for Wilkinson, given that this population is so vulnerable. Though anyone can contract and die from Covid-19, older Americans are more likely to develop severe cases due to their tendency to have an underlying health condition.
But Wilkinson said she refuses to give up hope on any patient — young or old. To help keep spirits high, Wilkinson learns about her patients and isn’t afraid to sing or dance. “Three Little Birds” is her go-to song, even if, as she jokes, she doesn’t always get the words right. “No one should die alone,” she said. “And that’s where we are right now, that people are not able to see their loved ones and we’re not able to do funeral arrangements.”
With so much uncertainty, there’s no telling what the future holds, but Wilkinson has already asked to be extended a few more weeks at Harlem Hospital. All she needs is approval from her full-time position in San Diego. And, as far as a return to normalcy, Wilkinson believes the country still has a long way to go — and cautioned about the potential repercussions of reopening the economy too soon.
“It might seem… calm, but in the hospitals, it’s not calm,” she said. “People are sick and they’re getting intubated and they are not coming out of it, and I feel that if we open the doors, the floods are going to come back in and we’re gonna be overwhelmed again in the hospitals.”
Written and reported by senior writer Tess Bonn.
This originally appeared on Medium.com