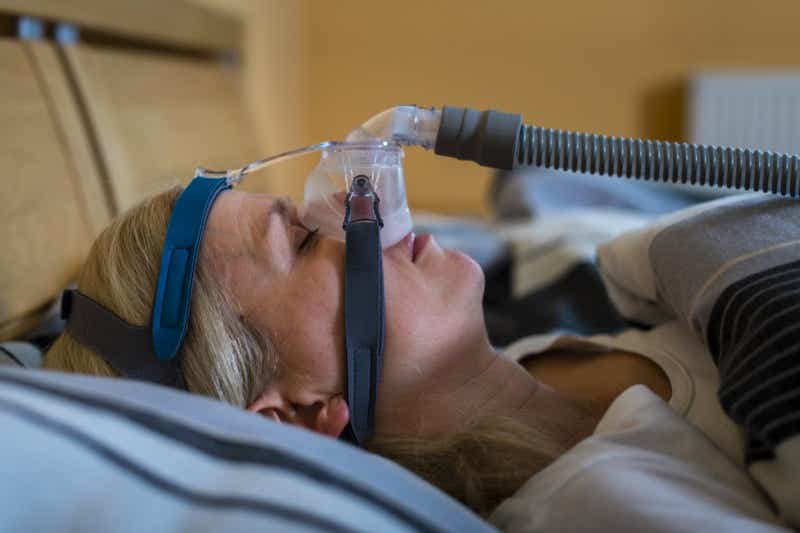
A group of engineers launched a new project to repurpose sleep apnea machines
For weeks now, we’ve been hearing about the shortage of ventilators and how it’s quickly become a national crisis. As doctors prepared to potentially make some very difficult decisions about these vital machines, a group of engineers and physicians working with UC Berkeley and UC San Francisco saw an opportunity to help. Knowing that many Americans with sleep apnea may have old CPAP or BiPAP machines in their homes, they decided to launch the Ventilator SOS Project. The initiative allows people to register and donate these machines, after which they will make the necessary adjustments to allow them to function in a hospital setting.
Our producer Emily Pinto spoke with Dr. Ajay Dharia, a Pulmonary Critical Care physician at Mills Peninsula Hospital and Bryan Martel, the managing director at Environmental Capital Group, about how this project could help hospitals right now.
Wake up Call: Tell us about the Ventilator SOS Project, and why you think the ventilator shortage could be alleviated by a machine that many of us might already have at home.
Dr. Dharia: With patients who have Covid-19, one of the main complications we’re seeing is that they’re not getting enough oxygen into their blood, and there are only a certain number of ventilators available. If Covid-19 gets worse, what do we do if we don’t have enough ventilators? That was the genesis of this idea. If there aren’t enough ventilators, can we offer people something that’s readily available that we can get out to hospitals in a number of weeks? We wanted to come up with a quick, easy solution that uses devices that were already out there.
CPAP (continuous positive airway pressure) and BiPAP (bilevel positive airway pressure) machines are currently in many people’s homes, usually used by people with sleep apnea. Our team is taking these machines from people’s homes, and they’re enabling them to be used similarly to hospital grade CPAP and BiPAP machines. There are modifications being made to make sure patients would get enough oxygen, because normal CPAP and BiPAP machines at home aren’t designed to provide high levels of oxygen support. Additionally, these home machines are designed to hook up to face masks, not to endotracheal tubes. So the team has come up with a solution to hook up these devices in a hospital.
Bryan Martel: What we need is a reservoir of these machines, so we’ve created a registry site for everyone in the country. As people register their machines, we can create a depository of these machines that are already built, and already working, and are already approved by the FDA for sleep apnea.
Then if a hospital or doctor wants to call on this registry, we will get the machines delivered. There are parts necessary to hook up the machine in the hospital, and we will try to get those parts — which we are calling a “pre-vent” box of parts — and those will go to the hospitals as well. Physicians will use these pieces to connect the CPAP or BiPAP machine to the endotracheal tube or to a mask.
These machines will give doctors an option when ventilators are used up, or they can take the load off of ventilators by being used before or after ventilator use. The doctors will have to make this call — we’re just trying to provide an option to doctors that we think is readily available. Right now people all over the country are registering their units. We have well over 1000 units now, and we are just trying to get the word out.
Which patients will be eligible to be put on these types of machines?
Dr. Dharia: The biggest challenge is going to be figuring out which patients will benefit the most from this. Knowing that exact patient population is not trivial — if someone is getting worse very quickly, they may need much more support than one of these machines can offer. So identifying the patient population will be the challenge for the clinician.
The two initial patient populations that we think would most benefit from a technology like this would be patients with more mild to moderate disease, because a home CPAP or BiPAP machine can offer higher levels of oxygen and pressure than traditional support mechanisms like a nasal cannula. The CPAP and BiPAP machines can elevate the pressure in the lungs, and we’ve seen clinically that Covid patients with lung disease respond well to pressure. So if we catch these patients with mild to moderate disease, we may be able to prevent intubation — prevent them from getting put on a full blown vent and saving that vent for someone who really needs it.
The second group of patients that I think could really benefit from this are people who have been on a vent for a while, and we’re trying to wean them off of it. So their lungs are improving, and they get to a point where they don’t need such high levels of support — they don’t need all of the mechanics and algorithms that you get from a ventilator. So you can transition them to a BiPAP or CPAP machine towards the end of their disease. Many patients right now are on ventilators for upwards of two weeks — that’s a really long time. So if we can reduce that to ten days, that extra four days will increase our effective ventilator pool by 30%.
But I want to be clear that this is absolutely a solution of last resort. We would prefer to have enough ventilators, or hospital-grade CPAP or BiPAP machines. But in the case we don’t, we’re trying to mobilize now so we can be ready if that happens.
Bryan: We engineers and logistics people are saying, here’s a solution. It’s low cost, it’s simple, and available. And we want to offer it to doctors to see if they can use it.
What is the main difference between a home CPAP or BiPAP machine and a ventilator?
Dr. Dharia: Well a ventilator is able to monitor and provide much more pressure than one of these machines, but there are other differences. For example, people on a CPAP machine have to be able to breathe on their own. So the breathing has to originate from patients themselves. The machine can provide extra oxygen and pressure, but you have to be taking big enough breaths by yourself, as opposed to a ventilator, where you can set it to have a person breathe X times per minute with X volume per breath. You can dial that in on a ventilator, but you can’t dial that in on a CPAP or BiPAP machine. So patients have to be conscious, and we can’t use as many sedatives or opiates because they blunt respiratory drive. And these things are correlated — as you get sicker and sicker, you need more assistance. So the ventilators would be oriented towards sicker patients, and these machines would be used for milder cases.
What are the downsides of using one of these machines?
Dr. Dharia: There are certainly downsides. Not every hospital is going to jump at this. The main risk with using a face mask as a non-invasive method — not just with CPAP and BiPAP machines, but also something called a high flow nasal cannula, which can give you a high amount of oxygen — is there’s a risk for aerosolization of the virus. So you have to be more careful. Usually people are put in a negative pressure room, meaning the air is being sucked out of the room and filtered. The people going into the room need to have proper PPE. I think a lot of that discussion has to be framed in the sense that if we have ventilators, we should be using them. But that conversation changes drastically when you have limited resources and you don’t have ventilators available. Then you might be willing to put on the PPE and treat the patient on a non-invasive machine, because you have no other option.
Bryan: What we’ve been trying to do is this: we are trying to provide thoughtful options for doctors during this national emergency. These options are not meant to replace ventilators, but they should be useful for doctors at their discretion. Hopefully these options will decrease the demand for ventilators, and possibly be useful when there are no ventilators left. The doctors will make this call.
What message do you have for anyone out there who might have an old CPAP or BiPAP machine in their home?
Bryan: We think you can help us. Please help us and other Americans. Go to ventilatorsos.com and register your unit. We will come and pick it up or get a box with bubble wrap sent to your home, so it can then be shipped to a hospital that requests the unit.
This interview has been edited and condensed.
This originally appeared on Medium.com